Videos and Text Contributors
Lauren McCormack
Ruchir Puri
John Roth
Emanuele Lo Menzo
Jon Gould
1.Introduction
This atlas is designed by the SAGES foregut committee to serve as a guide for those performing paraesophageal hernia repair. The intent of the atlas is to provide a description and visual guide of the critical steps of paraesophageal hernia repair. We intend to demonstrate several techniques that have been successful for the experts represented on the SAGES foregut committee. While no technique is adaptable to every situation, we hope to demonstrate a variety of perspectives for a challenging procedure.
The approach to the hiatus, whether performing a paraesophageal hernia repair, fundoplication or Heller myotomy are interchangeable. The SAGES VIDEO ATLAS: NISSEN has previously shown the below necessary steps in paraesophageal hernia repair.
1.PATIENT POSITIONING
2.TROCAR PLACEMENT
3.LIVER RETRACTION
We encourage you to find this text https://www.sages.org/foregut-video-atlas-demo/nissen-atlas/ to reference the above steps in the procedure. This atlas will focus on aspects of the hiatus that are unique and critical to paraesophageal hernia repair.
2.Reduction and Mobilization of Sac Contents
The stomach and any additional structures are carefully reduced through the hiatus using gentle retraction with atraumatic graspers until it cannot be reduced any further. Often, all the contents are not able to be reduced fully and will reduce with sac dissection. Oral gastric tube should be used to aid in gastric decompression.
Usually the short gastric vessels require division to gain access to the left crus and mobilize hernia sac contents. Division begins at the mid greater curve and is carried up to the angle of His. Division should be performed with an energy device.
3.Mobilization of the Hiatus and Reduction of Hernia Sac
The hiatus is initially approached from the left or right crus. The left is the most common. It is up to surgeon’s training and preference. Both crural dissections are necessary for the procedure.
LEFT CRUS DISSECTION
An assistant retracts the left crus laterally, exposing the edge of the hernia sac. Using an energy device, the edge of hernia sac is divided from the pleura off the crural edge and carried anteriorly. Alternating blunt and cautery dissection, the left side of the hernia sac is mobilized and separated from the mediastinal attachments. Gentle but firm inferior retraction on the sac is needed to reduce it while sweeping back mediastinal attachments.
RIGHT CRUS DISSECTION
The right gastro-hepatic ligament is opened exposing the right crus. The right crus is retracted medially while an assistant provides gentle lateral retraction of the lesser curve of the stomach. This exposes the right crus and edge of hernia sac. Using an energy device the hernia sac is divided from the crural edge. Sequential retraction and dissection is used to dissect hernia sac anteriorly to meet the left side. Care is taken to preserve the peritoneum overlaying the crura to strengthen crural closure.
REDUCTION OF THE HERNIA SAC
The hernia sac is then reduced with sequential retraction, blunt dissection, and with energy. With reduction of the sac, the remaining hernia contents will reduce into the abdomen. Fibrotic and recurrent hernia sacs can be tedious and difficult, which will require frequent transitions from left to right dissection. Care should be taken to preserve the Vagus nerves.
The pleura is often adherent to the hernia sac and care should be taken not to enter the pleural space. The pleura can be gently swept or pulled off the hernia sac. Should entry occur the opening should be enlarged to allow free flow of C02 to prevent tension capnothorax. Usually, patients tolerate capnothorax well but occasionally require reduction of insufflation pressure. Capnothorax should be released at the end of the procedure.
Next, posterior dissection can be completed. This will complete the dissection of the hernia sac from the mediastinum and release the phrenoesophageal ligament. Now that circumferential dissection and complete reduction of the hernia sac is completed. The hernia sac is often removed. The sac should be divided with an energy device, with care not to injury the GE junction, vagus nerves, esophagus or stomach.
4.Esophageal Mobilization
Circumferential esophageal dissection should be completed high into the mediastinum. Usually up to the level of the tracheal bifurcation. Dissection is performed with a combination of blunt and energy dissection. The thin connective tissue can often be bluntly dissected to reveal capillaries that require energy division. Now the hernia sac is reduced and the esophagus can be visualized, a penrose can be utilized to encircle the esophagus at the GE junctions to aid in gentle retraction. A 360 esophageal dissection is performed. The thoracic aorta is visualized but may be displaced to the right if the hernia was very large. Dissection should result in at least 2 cm of intraabdominal esophagus without tension. Usually dissection continues up to the level of the tracheal bifurcation. If additional length is necessary, a thoracic approach to mobilize the proximal esophagus or Collis gastroplasty will be necessary.
5.Hiatal Closure Techniques
Once adequate esophageal length has been obtained and all hiatal contents are fully reduced, it is time for hiatal closure. Closure should be performed posteriorly with non-absorbable suture. The assistant uses the Penrose drain to retract the esophagus anteriorly and to the left (3 o’clock position). Sutures area placed approximately 5 mm apart, starting posteriorly and working anteriorly. Closure options include interrupted or running non-absorbable suture with or without pledgets. Regardless of technique, it is important to incorporate peritoneum overlying the muscle. The final closure should have the hiatus in opposition to the esophagus but allow a grasper to avoid too tight of a closure.
6.Mesh Placement
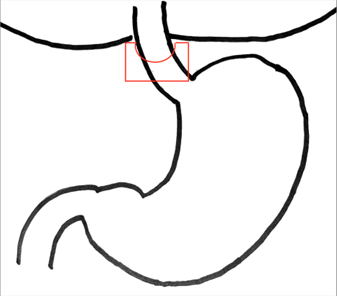
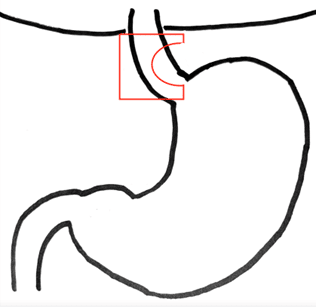
Mesh placement is controversial. It has shown to decrease recurrence in short follow up but no difference long term. Surgeons still utilize mesh for a variety of reasons including repair of recurrent hernias, attenuated crural muscle, poor or absent peritoneum and closure under tension. Biologic mesh should be used over synthetic. In Figure 1 you will see a variety of acceptable mesh placements in either a “U” or “C” configuration, the most common being the posterior placement with anterior gap. The mesh should not encircle the esophagus to prevent hiatal stenosis. Additionally, it should not be directly anchored to or have significant contact with the esophagus. Mesh is secured in place with at least three sutures, one at the base and at each arm. These practices help prevent mesh migration, erosion or hiatal stenosis. See Video 11 for placement of mesh at the hiatus.
7.Gastric Fixation
A form of intraabdominal gastric fixation is typically utilized to prevent future herniation and volvulus with hernia recurrence. This is accomplished with either gastropexy or fundoplication. Refer to SAGES VIDEO ATLAS: NISSEN for fundoplication, this Atlas will focus on gastropexy.
Gastropexy can be utilized in those patients who are not fundoplication candidates. Poor fundoplication candidates are most commonly those with poor esophageal motility or emergent settings.
Gastropexy sutures are typically placed from the fundus laterally to the left lateral diaphragm. Fixation is performed with permanent suture in either an interrupted or running fashion. An additional outflow fixation is performed from the antrum to the anterior abdominal wall. Anterior fixation can be performed with permanent suture in a transfascial or intra-abdominal fashion, another alternative is gastrostomy tube placement. Gastrostomy, is beneficial in patients who have anticipated delayed oral intake or post-operative gastroparesis. Gastrostomy is performed either laparoscopically or with a laparoscopic assisted PEG.
8.Challenging Considerations
A. The Short Esophagus
Ideally 2 cm or more of intra-abdominal esophagus is obtained during mediastinal dissection. This can usually be achieved with careful and thorough high mediastinal dissection of the esophagus. In rare occasions, the GE junction will remain at the level of the hiatus or above despite exhaustive mobilization. The shortened esophagus typically occurs in the setting of prolonged GERD, advanced PEH and congenital malformations. In these instances, there are several adjuncts to gain intra-abdominal esophagus.
Thoracic approach
If needed, consultation with thoracic surgery for proximal esophageal mobilization. This is planned preoperatively. Typically, thoracic mobilization is performed first followed by abdominal approach to finish dissection and perform crural closure.
Collis Gastroplasty
During Collis gastroplasty the stomach is tubularized to create a neo-esophagus. Transabdominally, a fundectomy is required. The fundus is divided lateral to medial, as proximal to the GE junction necessary to achieve intraabodminal neo-esophagus. After the initial transverse staple load, the remaining fundectomy should be performed with a bougie in place vertically toward the GE junction. It is required to use a bougie, a 52 Fr or greater is advisable. Continue to divide the stomach superiorly, staying generously off the bougie to the GE junction.
Steps
- Mobilize the esophagus until technically unable and determine that intra-abdominal esophagus cannot be achieved
- Measure the length of stomach needed to tubularize the stomach to obtain 2cm of intra-abdominal neoesophagus.
- Pass Bougie, at least 52 Fr, along lesser curve
- Begin fundectomy lateral to medial with appropriate staple load just distal to measured neo- GE junction.
- Finish Collis with transection parallel to Bougie with generous margin up to angle of His
- Remove partial gastrectomy specimen
- Proceed with crural closure and gastric fixation

B. Difficult Hiatal Closure
Difficult hiatal closure can be a challenge in the setting of recurrent hernias, fibrotic crural muscles and massive paraesophageal hernias. One options for crural closure is to perform a relaxing incision along the muscle. This can be done from the left or right sides
Right sided relaxing incision
The right diaphragm is divided in a vertical fashion just lateral to the right crus. It is important to identify the location of the IVC prior to division and knowledge its course so injury does not occur. Once the muscle is divided, the hiatus is closed. A mesh is used to prevent diaphgramatic hernia occurrence. Due to the presence of the liver, a biologic mesh is acceptable and can be used to also reinforce the hiatus.
Left sided relaxing incision
Left sided relaxing incisions are less common due to the lack of solid organ procession to prevent diaphragmatic hernia but are used per surgeon preference. The left diaphragm is divided in a vertical fashion just lateral to the left crus, in the same manner presented for the right side. Once the muscle is released, the hiatus is closed in a standard fashion. As there is no solid organ protection along the left diaphragm a permanent coated mesh is needed to cover the relaxing incision defect.